How the Increase of Men in Memory Care is Changing the Industry
New data by A Place for Mom reveals that over the past three years, male move-ins to memory care are growing at a rate that is 14% greater than women. Learn more about this new insight and what it means for your community.

Why It’s Happening and What It Means to You
If I use the words “demographics” and “senior care” together, I bet your mind immediately goes to the growing numbers of Boomers who are exiting the workforce and entering senior living. This is a very important demographic trend for our industry, but it isn’t the only one that matters.
Two times more women than men move into memory care, but men are catching up.
Alzheimer’s disease tends to affect a disproportionately large number of women. According to the Alzheimer’s Association, nearly two-thirds (65%) of people over the age of 65 who are suffering from Alzheimer’s in the U.S. are women. A Place for Mom’s historical data backs up this 2:1 female to male ratio. However, recent data suggests that the trend is beginning to change.
A Place for Mom’s figures show that move-ins by men to memory care communities are increasing 14% faster than women over the past three years. Our partner communities have reported significant influxes of male residents, sometimes two to five times as many male inquiries compared to just a few years ago.
“While women continue to be diagnosed with Alzheimer’s Disease at a higher rate, we are seeing a significant increase in men seeking memory care with the number of our male residents doubling in the past 18 months,” said Megan Carnarius, RN and Executive Director for Balfour Cherrywood Village, an Alzheimer’s and memory care community located in Louisville, CO. “The prevalence of the disease in more people could be attributed to more people living longer. The older you get, the higher chance you have of getting the disease, and men specifically are living longer.”
When families inquire about a male senior, they are more likely than women to move into memory care. Data over the past year shows that when males inquire about senior care with A Place for Mom, they are 27% more likely than women to require memory care services.
Of the people that move into licensed care with A Place for Mom, 27% of men require memory care services versus 21% for women.
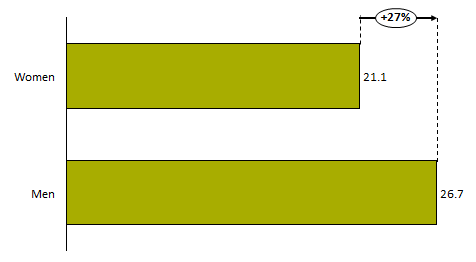
Percent of Licensed Care Move-Ins that Include Memory Care Support
Why Are More Men Moving to Memory Care?
A Place for Mom’s research suggests two factors are causing growing numbers of men to move into memory care:
1. Shrinking Age Gap
Women tend to live longer than men, but the gap between the two is gradually shrinking. Both genders are living longer, but the male average lifespan is increasing faster than that of women. Male life expectancy increased 6% in the past 25 years, which is twice the rate of women. Experts have pointed to a number of factors driving this trend, including fewer wars, reduced risky behavior like smoking, lower propensity for obesity and better treatment of gender-specific diseases. Higher life expectancies mean men have a higher likelihood to live long enough to require Alzheimer’s or dementia care. This is a key factor driving the gender difference of memory care populations which explains most of the difference.
2. Acute Health Problems
When men and women reach out to A Place for Mom, they are not equally likely to display symptoms of memory diseases. Men are 8% more likely to exhibit wandering tendencies and 30% more likely to have issues with combative behavior. Combativeness can force the transition to memory care. Evan DuBro, CEO of Our Family Home, notes that it can be more difficult for wives and daughters to be caregivers to the end. Men are likely to be bigger and stronger than women, in addition to being more likely to exhibit combative behavior. Frequent agitation complicates caregiving and can speed the transition to professional memory care.
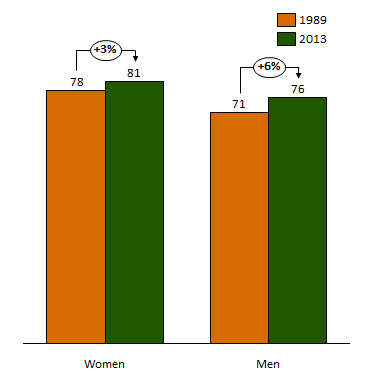
Average Life Expectancy by Gender
What This Means for Memory Care Communities
When we speak to partner properties about gender and memory care, they are quick to point out their focus on tailoring care to each individual resident. This is a sound approach, but it shouldn’t prevent awareness about differences between male and female residents. Increasing numbers of men living in memory care communities has implications for providers.
Memory care providers that partner with A Place for Mom shared some examples of how they are making changes to care practices in response to the increase of men requiring memory care.
These include:
1. Expanding Features Tailored Towards Men
This fast-moving trend has important implications for the management of memory care communities. Juliet Holt Klinger, VP of Dementia Care at Brookdale, notes that their communities have been adding more male-oriented spaces like work benches, military reminiscing areas, and sports areas. Of course these features aren’t the exclusive domain of men, but they can be effective marketing tools for prospective male residents and great for keeping existing male residents engaged.
2. Finding New Ways to Engage
Men’s interests are sometimes different than women and it’s important that caregivers get to know each person to understand their backgrounds, past careers, and their interests. This helps to identify what they are accustomed to doing on a daily basis, which facilitates engagement. One clever caregiver at HCR Manorcare learned that a memory care patient used to referee their high school football games. When the resident would get agitated, the caregiver would call over and say, “Hey Joe, I want to talk with you about that game where I threw three interceptions.” It calmed him down every time.
3. Knowing How to Diffuse Aggressive Behavior
Men are usually physically larger and stronger than women, and even aged men can be quite strong. Senior care staffs generally skew female, which means staff should be trained to manage and diffuse triggers of aggressive behavior. Caregivers at Brookdale are trained to approach caregiving as a partnership with the resident, versus “you are in my care and I’m going to tell you what to do.” The former attitude empowers the resident, which helps maintain self-esteem.
4. Encouraging Independence When Possible
Men often are very proud and don’t like having help, especially for simple tasks like shaving that they’ve been doing independently for decades. Finding and empowering seniors to do activities they can do on their own as much as possible is important. Kristin DuPont, Director at the LaSalle Group, told the story of a resident that came to the dining room but wouldn’t eat, claiming that it was “just too much food.” They would serve smaller portions but that didn’t work, and the staff was worried that he wouldn’t get enough to eat. The Chef had the idea to put the same amount of food on a large platter. The portion looked much smaller so he ate it.
5. Expecting Quicker Move Timelines
Males’ higher likelihood to be combative and wander suggests that their health needs are more acute when their loved ones reach out for help on their behalf. More acute health needs mean that you can expect a shorter length of time between inquiry and move-in. A Place for Mom asks every family we speak to about when they expect to move. Families of male seniors have a greater of urgency on average. Loved ones of male prospective residents are 43% more likely to expect to move within 7 days, and 17% more likely to expect to move within 30 days.
Does your community have amenities that are catered to men? Please share your ideas in the comments below.






Hello Nick,
Great article. I’m the Executive Director for an Assisted Living and Memory Care Community in Keller, Texas. Our memory care offers 23 private suites and 8 of our 23 residents are men. We have taken them to the putting green nearby for golfing, and offered croquet on the lawn here. We also have raised garden beds which they enjoy and also a monthly Veteran’s Lunch. Having so many men in the Memory Care is actually a real plus and definitely changes up the dynamics. You can view our golfing outing at http://www.youtube.com/watch?v=ZI3ckjRTCXE
Have a blessed day,
Jamie Bryant
Thanks for posting this! When I opened Angel House, my small south Florida ALF home and APFM partner, it was in response to my experience with my own dad and the need I saw for men, especially veterans.
My dad was very strong and independent, but died fearing death Less than he feared a nursing home… That very sad fact led me to the awareness that Assisted Living is very different than traditional nursing home care, and then to the community need we help to fill today.
Our home has very individual activities, but also very “normal” ones. We have live music and Residents dance. In our small 6-bed ALF, we have only one to 2 men as a rule, for the traditional reasons cited. That man (or 2) can be very busy and in demand as a dance partner! Another I would add is that men typically don’t want to share a room, and in the small setting, this is more problematic, especially with today’s budget constraints and general economy.
Often, when someone’s been in AL care for a few years, families move them to smaller homes, so they can get more individual care. And men resist care outside the home longer, all other things being equal. They want to stay home, and thus they may become more critically or acutely frail Before they accept a move. Then the move, sadly, is to a Skilled Nursing Facility rather than one of the lovely APFM partner ALF homes in our community.
Our community is very diverse, in that we have many Hispanic residents, most of them to varying degrees, bilingual. I myself, grew up in Central America, so I’m fully fluent in both English and Spanish. Studies show that maintaining a second language slows cognitive decline significantly. This is because the brain gets more exercise when translating/switching languages, maintaining cognition.
Our small bilingual care home really is a great model for quality of life, in our aging and culturally rich south Florida, with outings, live music and a great caregiver to Resident ratio that provides for the “only” man or two men, to experience greater fulfillment and thus, less anxiety, which leads to less combativeness overall.
Even small details, like being sure they always have “their own” chair, and a place at the end of the table, can make a big difference in their self-esteem. So much is taken out of their control as people age, that they really need to feel loved and respected, and in control of at least some areas of life.
In short, we try to treat every man like the beloved father we have or that we lost. This truly means quality of life, and is our mission.
My own Daddy had already passed away by the time I began to work toward opening Angel House, but it lives as a legacy to him and to warm, caring family style care in a very diverse community.